New Research Reveals Impact of High-Quality Ventilation During CPR and Need for Improved Techniques
Study Shows Three-fold Increase in Survival Rates for Out-of-Hospital Cardiac Arrest Patients Who Received Optimal Ventilation
Current resuscitation guidelines for first responders recommend pausing after every 30 compressions to provide ventilation, then delivering two breaths using a bag valve mask (BVM). This is known as 30:2 CPR.
A recent multicenter study, partly funded by the National Institutes of Health and published in the American Heart Association’s Circulation newsletter, sought to measure the quality and frequency of bag-valve-mask ventilation during 30:2 CPR. The study aimed to uncover the extent to which lung inflation occurred in out-of-hospital cardiac arrest patients and the resulting outcomes.
Leading the charge, Dr. Ahamed Idris, Director of Emergency Medicine Research at the University of Texas Southwestern Medical Center in Dallas, expressed the significance of the study stating, “This is one of the first studies to measure the quality and frequency of ventilations used during CPR. While we suspected that better ventilation was going to show some benefit to patients, the result that we got was much more than we expected. It was very surprising.”
The findings were clear. Patients experiencing out-of-hospital cardiac arrest who received more frequent and higher-quality ventilation during the compression pause experienced significantly better clinical outcomes.
- A threefold increase in survival rates (13.5% vs 4.1%)
- A higher rate of resuming a sustained heart rhythm (40.7% vs 25.2%)
- Improved neurological outcomes with a lower probability of brain damage (10.6% vs 2.4%)
However, the study revealed that 60% of patients did not receive consistent, high-quality ventilation. Researchers identified several first responder techniques that contributed to this:
- Failure to measure ventilation when using a BVM
- Inadequate opening of the airway
- Insufficient prevention of mask leaks
Acknowledging the challenges associated with efficient BVM ventilation, researchers emphasized the need for continuous practice and suggested that agencies should provide responders with tools to accurately measure ventilation when using a BVM.
The research underscores the importance of high-quality ventilation during CPR, highlighting the significant impact it can have on the lives of out-of-hospital cardiac arrest patients.

EOlife X: The Ultimate Training Tool for High-Performance Ventilation
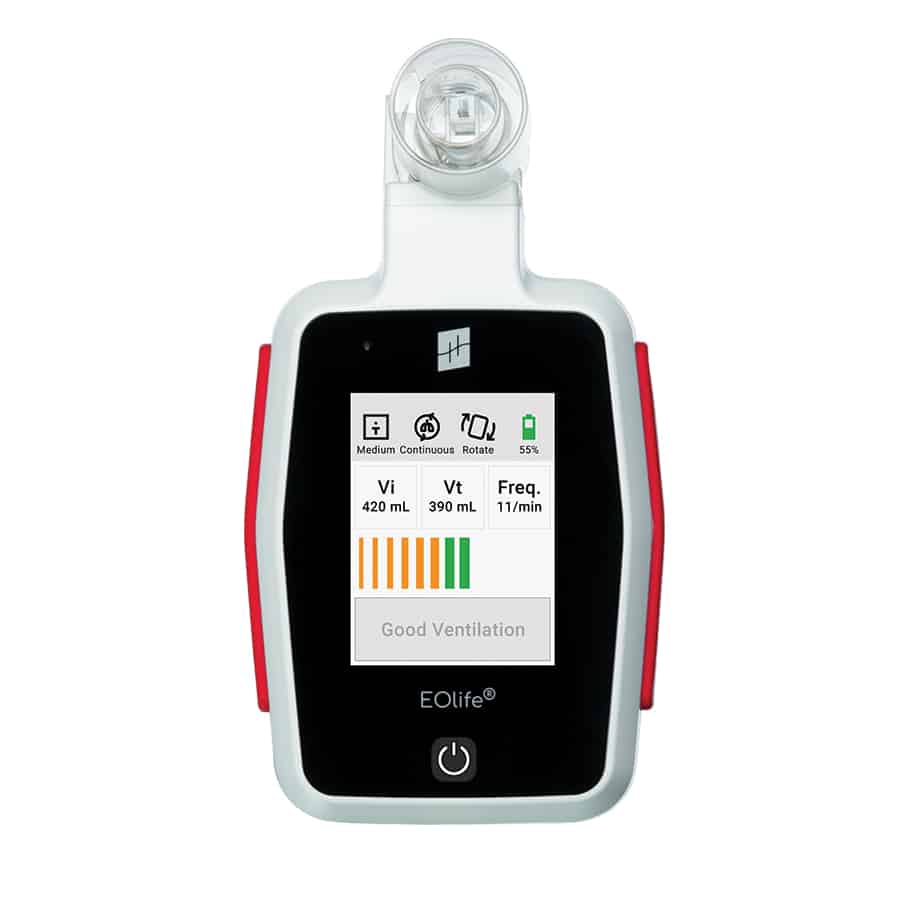
EOlife: The Ultimate Feedback Device for High-Performance Ventilation
EOlife X teaches first responders about proper airway management and good ventilation regardless of the user’s level of experience and patient profile. With adult and pediatric settings, the device provides visual feedback on the quality of ventilation with two training modes (blind or monitored) that record ventilation parameters. Data can be downloaded via Bluetooth to the EOlife Connect app which offers detailed analysis and allows users to track their skills progress over time.
EOlife is an FDA-cleared, reliable and intuitive medical device that measures ventilation parameters and can provide users with real-time feedback on the quality of manual ventilation to the patient. EOlife offers two different user interfaces depending on the type of user (ALS or BLS). By providing visual feedback, the device increases the quality of manual ventilation by 70%, reduces the risk of hyperventilation tenfold and can double the chance of patient survival.
For more information and to request a demonstration of EOlife X and EOlife, call 888-891-1200 or email us to be connected to your local sales representative.
MED Alliance Group is a medical device distributor that has been meeting the needs of our clinical customers and manufacturing partners since 1998. We specialize in the sales, marketing, importation, logistics and distribution of innovative, high-quality and cost-effective products found in anesthesia and respiratory, blood and transfusion therapy, EMS and emergency room, interventional radiology and cath lab, iv and vascular, as well as NICU and PICU.
Please follow us on LinkedIn, Facebook and Twitter for MED Alliance product updates.